65 Y Old female came to casualty with C/O fever since 4 days,Shortness of breath since 2 days,pedal edema since 2 days,OSA since 8 months
202351350
202355137
November 10,2023
This is an online e log book to discuss our patient de-identified health data shared after taking his / her / guardians signed informed consent. Here we discuss our individual patients problems through series of inputs from available global online community of experts with an aim to solve those patients clinical problem with collective current best evident based input.
This E blog also reflects my patient centered online learning portfolio and your valuable inputs on the comment box is welcome.
I have been given this case to solve in an attempt to understand the topic of " patient clinical data analysis" to develop my competency in reading and comprehending clinical data including history, clinical findings, investigations and come up with diagnosis and treatment plan
Cheif complaints
65 Y Old female came to casualty with C/O fever since 4 days,Shortness of breath since 2 days,pedal edema since 2 days.
Past and present history:-
This is a case of 65 year old female resident of nagarjuna sagar presented to casuality with above complaints.
Pt wa lols born and brought up in nagarjuna sagar and studied up to 10th standard.Was married at the age of 17years and had two female children at the age of 18 and 21 years.
Her husband was a lorry driver and 20 years back he met with RTA and expired.She was worried about her husband death and gradually it effected her daily routine.she started to consume more than required to deviate her mind from husband demise and started to gain weight.she was apparently asymptomatic till 10 years ago and developed neck pain and headache for which she went to hospital and diagnosed of having htn and started on antihyoertensives(tab.telma 40 and metxl trio) and till 3 years back she remained asymptomatic and then developed generalised weakness,polyuria and polydysia for which she was diagnosed of having DM2 and started onOHA's which later converted to inj.mixtard as her sugars remain uncontrolled with OHAs.In 2020 she develeoped chest pain o acute onset and CABG was done i/v/o CAD and since january 2023 she is having sob and pause of breaths during sleep and diagnosed of having OSA and was on intermittent bipap at home
Present illness:-4 days back she develeoped fever of highgrade intermittent relieved of medication and 2 days ago she developed pedal edem(b/l) and pain iver dorsum of rt foot for which hot compressions were applied and sob of grade 2 since 2 days not associated with cough,palpitations,chestpain ,profuse sweating
Past illness in brief:-
K/c/o htn since10 yrs on tab.telma 40 and tab.met xl trio
K/c/o DM2 since 3 years and on injj.mixtard sc. bd
K/c/o CAD s/p CABG in 2020
K/c/o OSA Since jan 2023
General examination
Pt is c/c/c
Pallor +
B/l pedal edema +
No icterus cyanosis clubbing lymphadenopathy
Ulceration over dorsum of rt foot+
Temp afebrile
Bp 150/80 mm hg
Pr 86 bpm
Rr 18cpm
Systemic examination
Cvs : s1 s2 heard no murmurs
Cns:nfnd
Rs:Blae+Nvbs
P/A: soft non tender
Ht:-5.4/wt:- 120 kgs
pulmonology referral was done i/v/o cough and sob they adviced tab. Acebrophylline 100mg bd
Nebs ith ipravent 6th hrly budecort 8th hrly
Tab pcm 650 tid
O2 inhalation 1to 2lt/min to maintain spo2 above 95%
Surgery refrl was taken I/V/O RT LOWER LIMB CELLULITIS, BEDSORE,GANGRENE OF 5TH TOE
TREATMENT- TAB . CHYMEROL FORTE 10MG PO TID
MGSO4 +GLYCERINE DRESSING, AIR BED
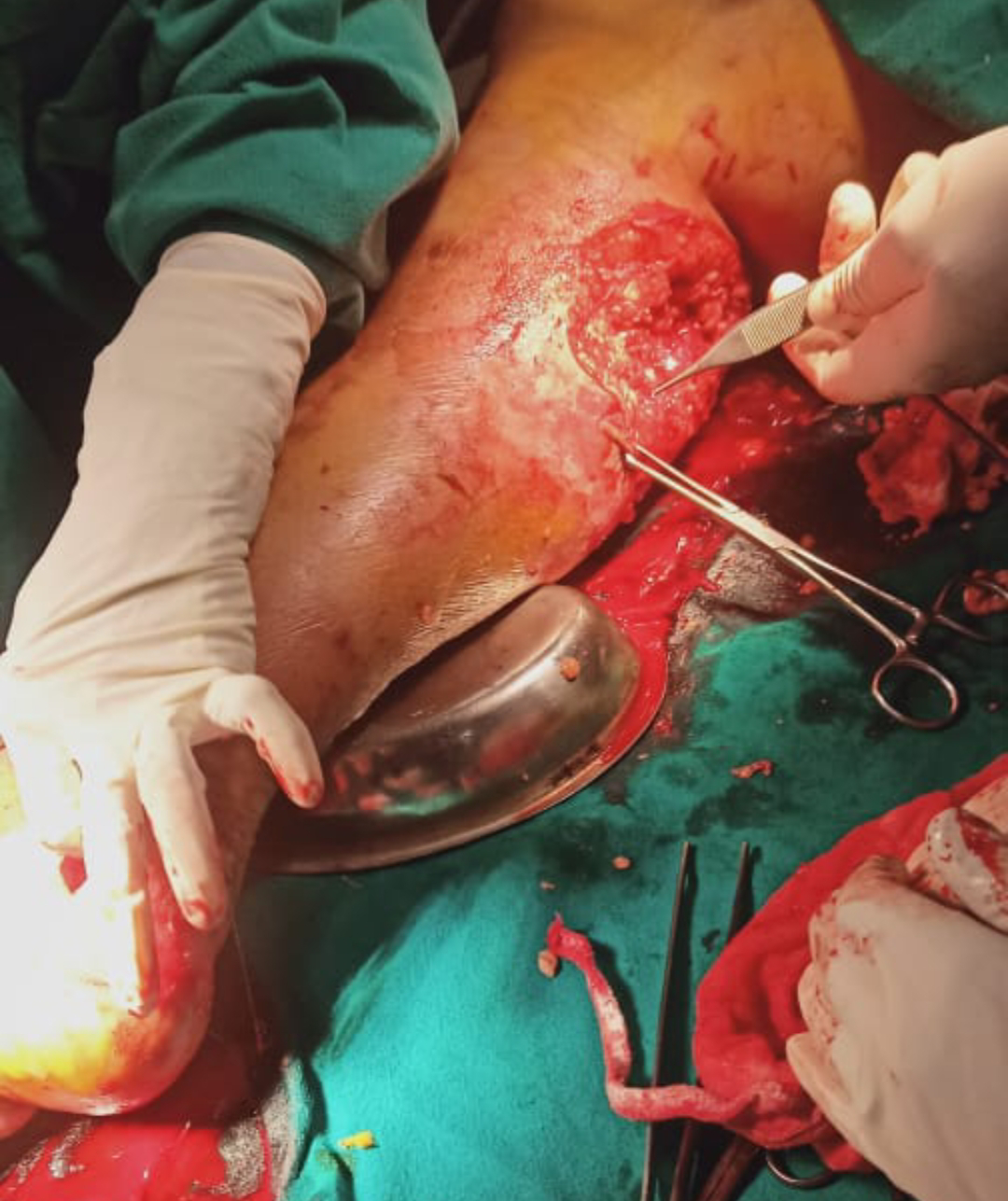
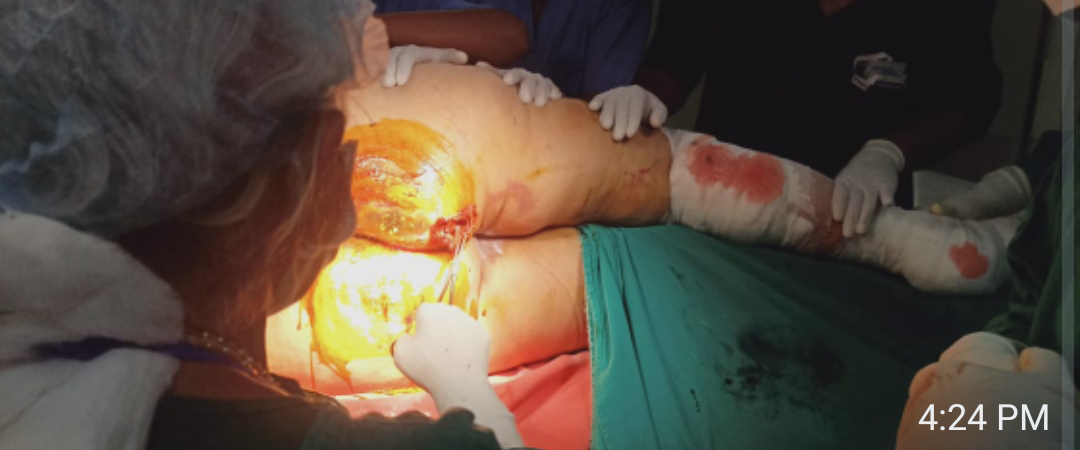
DISARTICULATION OF RIGHT5 TH TOE WITH DEBRIDEMENT OF ULCER AND BEDSORE UNDER SA DONE ON 24/11/23
DVL REFERRAL I/V/O ITCHY SKIN LESIONS OVER GROIN AND INNER THIGHS
TREATMENT- CLOTRIMAZOLE 1% CREAM L/A BD X 1 WEEK
ABZORB DUSTING POWDER L/A BD X 2 WEEKS
COURSE IN THE HOSPITAL-
A 65 YR OLD FEMALE PRESENTED WITH C/O FEVER SINCE 4 DAYS, SHORTNESS OF BREATH SINCE 2 DAYS, PEDAL EDEMA SINCE 2 DAYS,
SOB GRADE III AND ON FURTHER INVESTIGATIONS DIAGNOSED WITH TYPE II DIABETES MELLITUS ,HYPERTENSION .K/C/O CAD S/P CABG IN 2020,
ACUTE KIDNEY INJURY ,GANGRENE OF 5TH TOE, ULCER OVER DORSUM OF FOOT & RT CALF,GRADE II BEDSORE OF B/L GLUTEAL REGION S/P DISARTICULATION OF 5TH RT TOE & DEBRIDEMENT OF ULCER & BEDSORE UNDER SA ,CANDIDIAL INTERTRIGO +FRICTIONAL DERMATITIS.
S/P 9 SESSIONS OF HEMODIALYSIS DONE , 4 BLOOD TRANSFUSIONS DONE
PATIENT IS MANAGED CONSERVATIVELY WITH ANTIBIOTICS AND PLANNED FOR DISCHARGE
Investigations
Diagnosis:-OBSTRUCTIVE SLEEP APNEA
HEART FAILURE W/ PRESERVED EJECTION FRACTION (EF=65%)
ULCER ON THE DORSUM OF THE RIGHT FOOT
GRADE III BED SORE ON B/L GLUTEAL REGION
CANDIDA INTERTRIGO + FRICTIONAL ULCERS ON INNER SIDE OF THE THIGHS
PRERENAL AKI ON CKD
ANEMIA OF CHRONIC DISEASE
PULMONARY HYPERTENSION TYPE III
DM II + HTN
S/P AMPUTATION OF 4TH AND 5 TH TOE OF THE RIGHT FOOT
S/P PTCA 2015 + S/P CABG 2020
S/P 9 SESSION OF HEMODIALYSIS
4 PRBC TRANSFUSIONS.
4 FFP TRANSFUSIONS
TREATMENT GIVEN O2 INHALATION TO MAINTAIN SPO2 >95% BIPAP FOR 18 HRS
INJ MOXIFLOXACIN 400MG IV OD 8AM
INJ METROGYL 500MG IV 8TH HRLY
INJ LINEZOLID 600MG IV 12TH HRLY
INJ MEROPENEM 1GM IV 12TH HRLY
INJ HYDROCORTISONE 100MG IV PRIOR TO DIALYSIS
INJ PANTOP 40 MG IV BBF
INJ LASIX 40MG IV BD
INJ PCM 1G IV IF TEMP > 101F
TAB PCM 650MG PO 8TH HRLY
TAB ATORVASTATIN 40MG RT/OD
TAB ACEBROPHYLLINE 100MG RT/12TH HRLY
TAB NODOSIS 500MGRT 8TH HRLY
TAB SHELCAL CT RT OD
TAB OROFER XT RT OD
INJ HUMAN ACTRAPID INSULIN SC/PREMEAL 12U
ABSORB DUSTING POWDER LA BD
COTRIMAZOLE 1% CREAM LA BD
RT LOWER LIMB ELEVATION
REGULAR POSITION CHANGING 2ND HRLY
ALPHA BED
TAB AMLONG 5MG PO OD
TAB ECOSPRIN 75MG PO OD
TAB CLOPIDOGREL 75MG PO OD.
ADVICEAT DISCHARGE TAB LEVOFLOXACIN 500MG PO BD X 7 DAYS
TAB AUGMENTIN 625MG PO BD X 7 DAYS
TAB CEFIXIME 200MG PO BD X 7 DAYS
TAB ATORVASTATIN 40MG RT/OD X 10 DAYS
TAB ACEBROPHYLLINE 100MG RT/12TH HRLY X 5 DAYS
TAB NODOSIS 500MG PO X 5 DAYS
TAB SHELCAL CT RT OD X 15 DAYS
TAB OROFER XT RT OD X 15 DAYS
TAB PCM 650MG PO SOS
TAB AMLONG 5MG PO OD X 10 DAYS
TAB ECOSPRIN 75MG PO OD X 5 DAYS
TAB CLOPIDOGREL 75MG PO OD X 5 DAYS
ABSORB DUSTING POWDER LA BD
COTRIMAZOLE 1% CREAM LA BD
RT LOWER LIMB ELEVATION
REGULAR POSITION CHANGING 2ND HRLY
ALPHA BED.
Next admission:- on 9/12/2023
NEXT ADMISSION ON 9/12/23_COMPALINT OF SOB SINCE 5 HOURS
PT IS K/C/O OF OBSTRUCTIVE SLEEP APNEA W/ HTN / DM II WITH ULCER ON DORSUM OF RIGTH FOOT W/ GRADE III BED SORE , AMPUTATION OF 4TH AND 5TH TOES OF RIGHT FOOT WITH CKD WITH S/P 9 SESSIONS OF HEMODIALYSIS , 4 PRBS TRANSFUSIONS W/ CANDIDA INTERTRIGO ON INNER SIDE OF THIGHS.
HOPI: PATIENT WAS APPARENTLY ASYMPTOMATIC 5 HOURS BACK THEN SHE DEVELOPED SOB WHICH WAS INSIDIOUS IN ONSET GRADUALLY PROGRESSIVE, NOT RELIEVD WITH REST, GRADE III MMRC.
NO H/O CHEST PAIN, PALPITATION, SYNCOPE, HEADACHE, FEVER, VOMITING, LOOSE STOOLS.
NO H/O PAIN ABDOMEN, BURNING MICTURITION.
PAST HISTORY: K/C/O DM II SINCE 15 YEARS NOW ON MEDICATION INJ HAI 14U ----- 14U ---12 U
K/C/O HN SINCE 10 YEARS ON MEDICATION TAB TELMA 40 MG , TAB MET XL TRIO
K/C/O OBSTRUCTIVE SLEEP APNEA SINCE 11 MONTHS ON INTERMITTENT BIPAP SUPPORT
PAST HISTORY OF ULCER ON DORSUM OF THE RIGHT FOOT FOR WHICH DEBRIDEMENT AND FASCIOTOMY WAS DONE.
4TH AND 5 TH TOES OF THE RIGHT FOOT WERE AMPUTATED.
K/C/O CAD- S/P, CABG IN 2020
PERSONAL HISTORY:
DIET: MIXED
APPETITE: NORMAL
SLEEP: ADEQUATE
BOWEL AND BLADDER: REGULAR
ADDICTION: CHRONIC ALCOHOLIC SINCE 15 YEARS
GENERAL EXAMINATION:-
PATIENT IS CONSCIOUS, COHERENT, COOPERATIVE
BP:- 120/80 MMHG
PR:- 100 BPM
RR:- 20CPM
GRBS:- 208 MG/DL
TEMPERATURE:- 101 F
SPO2:- 97% @RA
CVS:- S1S2 HEARD,NO MURMUR
RS:- BAE PRESENT, NVBS
P/A:- SOFT, NON TENDER
CNS:- NO FOCAL NEUROLOGICAL DEFICITS
DEATH SUMMARY
THIS IS A CASE OF 65 YR OLD FEMALE FROM NAGARJUA SAGAR , HOUSEWIFE BY OCCUPATION, WHO IS K/C/O OBSTRUCTIVE SLEEP APNEA W/ HEART FAILURE W/ PRESERVED EJECTION FRACTION W/ ANEMIA OF CHRONIC DISEASE , PULMONARY HYPERTENSION TYPE III , ULCER ON DORSUM OF RIGHT FOOT W/ GRADE I BED SORE W/ DIABETES MELLITUS TYPE II W/ HYPERTENSION W/CKD . S/P PTCA IN 2015 , S/P CABG IN 2020 W/ 9 SESSIONS OF HEMODIALYSIS W/ S/P DEBRIDEMENT OF RIGHT FOOT W/ AMPUTATION OF 4TH AND 5TH TOES OF RIGHT FOOT . PREVIOUSLY ADMITTED UNDER US FOR SHORTNESS OD BREATH FOR 25 DAYS AND ULCER ON DORSUM OF RIGHT FOOT . PT WAS DISCHARGED FROM OUR HOSPITAL W/ HOME OXYGENATION SUPPORT AND WAS ON CONSERVATIVE MANAGEMENT W/ INTERMITTENT BiPAP SUPPORT . PT WAS ADMITTED IN DISTRICT HOSPITAL FOR OXYGEN SUPPORT. PT WAS MAINTAINING SP02 96% ON 2-3 LITRES OXYGEN SUPPORT . SHORTNESS OF BREATH AGGRAVATED SUDDENLY FOR 2 HRS AND OXYGEN REQUIREMENT INCREASED UPTO 6-8 LITRES AND PT CAME TO OUR CASUALITY FOR FURTHER MANAGEMENT.
AT THE TIME OF ADMISSION, BP - 120/80 MMHG , PR-100BPM , RR-20CPM , TEMP -101F , GRBS-208 MG/DL , SP02 - 80% ON RA , 97% ON 4 LIT O2 . ABG SHOWED - PH -7.364 , PC02 -48.1 , P02 -44.6 , HC03 -26.7 , HB-7.6 , TLC - 9600 , PLTS-4.5 LKHS, CREAT-1.7 , UREA -70 . PT WAS MAINTAINED ON INTERMITTENT CPAP AND BIPAP SUPPORT . FOLLOWING ADMISSION , BED SORE HAS PROGRESSED FROM GRADE II TO GRADE III. AFTER SENDING BLOOD AND URINE CULTURES , IV ANTIBIOTICS WERE STARTED AFTER 5 DAYS OF ADMISSION. PT HAS INTERMITTENT FEVER SPIKES THROUGHOUT THE DAY , IV ANTIBIOTICS WERE ESCALATED. 2D ECHO REVEALED PULMONARY ARTERY HYPERTENSION FOR WHICH CONSERVATIVE MANAGEMENT WAS GIVEN . REGULAR DRESSINGS WERE DONE FOR ULCER ON DORSUM OF RIGHT FOOT AND STARTED MUCIPROCIN OINT FOR SCAB ON THE BEDSIDE . 2 PRBS TRANSFUSIONS WERE DONE FOR CORRECTION OF ANEMIA , 1 INJ ALBUMIN 20% IV STAT; CORRECTION WAS DONE I/V/O LOW SERUM ALBUMIN AND PROTEIN RICH DIET WAS ADVISED . AS COAGULATION PROFILE WAS DERANGED aPTT-55 S, PT-26 S, INR-1.9 , 4 FFP TRANSFUSIONS WERE DONE AND INJECTION VIT K WAS GIVEN.
PT WAS MAINTAINED ON INTERMITTENT CPAP SUPPORT SINCE ADMISSION. ON 19/12/23 , ABG SHOWED PH-7.2 , PCO2 -66.4 , P02 -80 , HCO3- -25.5 , S02 -95.5 . AS THE PT STARTED DEVELOPING TYPE II RESPIRATORY FAILURE . PT WAS KEPT ON CONTINUOUS CPAP SUPPORT THROUGHTOUT THE NIGHT EVEN AFTER WHICH CO2 RETENTION WAS PRESENT . PT WAS INTUBATED AND CONNECTED TO MECHANICAL VENTILATOR . ON THE NEXT DAY, PT WAS KEPT ON ACMV-VC MODE ON FiO2 60. 4 HRS AFTER INTUBATION THERE WAS A DROP IN 02 SATURATION . PULSE AND BP WERE NOT RECORDABLE CPR WAS INITIATED ACCORDING TO LATEST ACLS GUIDELINES AND WAS CONTINUED UPTO 30 MIN . INSPITE OF ABOVE RESUSCITATIVE EFFORTS PT COULD NOT BE REVIVED AND WAS DECLARED DEAD AT 12:10 PM AS THE ECG SHOWED FLATLINE.
IMMEDIATE CAUSE OF DEATH:- TYPE II RESPIRATORY FAILURE
ANTECEDENT CAUSE OF DEATH:- OBSTRUCTIVE SLEEP APNEA , HEART FAILURE WITH PRESERVED EJECTION FRACTION , ULCER ON DORSUM OF FOOT , GRADE II BED SORE (B/L GLUTEAL) , ANEMIA OF CHRONIC DISEASE , CKD, PAH, DM II , HTN.
Outcome:- mortality
https://mvineelarollno90.blogspot.com/2023/11/65-y-female-with-co-fever-since-4-days.html?m=1




<< Home